If you are dealing with symptoms like these, it is easy to feel confused or dismissed.
- Shortness of breath that does not make sense.
- Constant fatigue even after a full night of sleep.
- Chest pressure that feels serious but tests keep coming back normal.
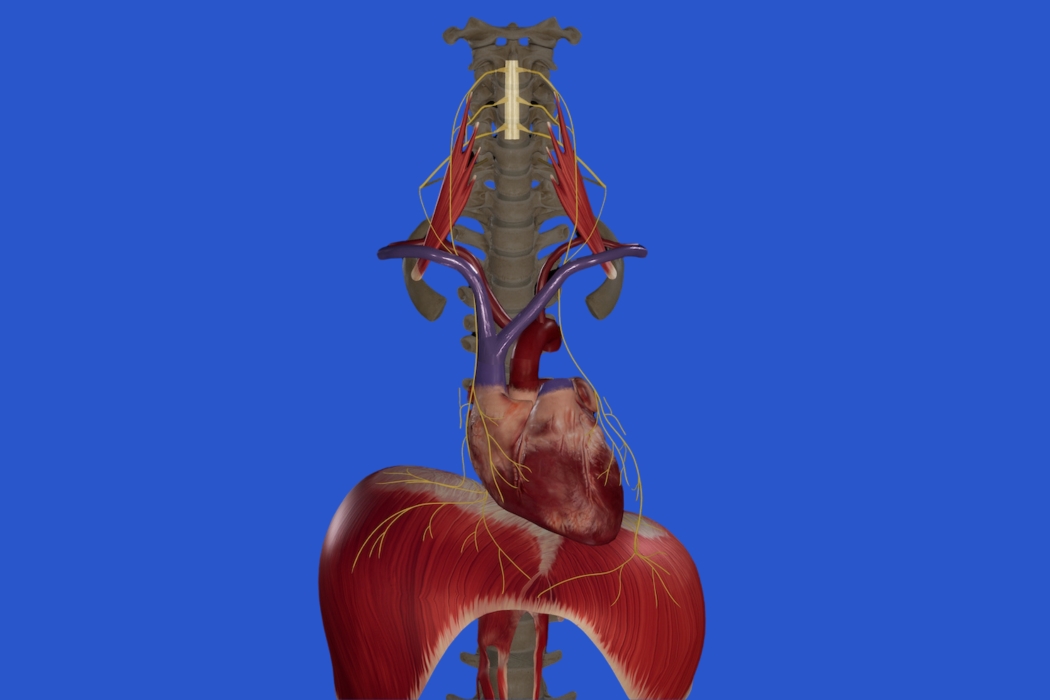
Breathing is not just about your lungs. It depends on proper nerve signaling. Your brain sends electrical messages through specific nerves that tell your diaphragm when to contract and relax. If that signal is disrupted, your breathing can feel off even if your heart and lungs are technically healthy.
One of the most important nerves involved in breathing is the phrenic nerve. When this nerve is irritated, compressed, or damaged, the diaphragm may not move the way it should.
Because most doctors first look at the heart and lungs, nerve-related breathing problems are often misdiagnosed as anxiety, asthma, or general deconditioning.
If you are experiencing complex or unexplained nerve-related symptoms, working with a specialist matters. Dr. Shane Huch, a pain management specialist in New Jersey, evaluates nerve-driven conditions that are often overlooked.
What is the Phrenic Nerve?
The phrenic nerve starts in your neck. Specifically, it comes from the C3 to C5 nerve roots in the cervical spine. A simple way to remember it is: C3, 4, 5 keep the diaphragm alive.
What It Does
The phrenic nerve controls the diaphragm. The diaphragm is the large dome-shaped muscle that sits under your lungs. Every time you inhale, the diaphragm contracts and moves downward, creating space for your lungs to expand and fill with air.
Without a properly working phrenic nerve, that contraction becomes weak or absent.
One Side vs Both Sides
You have two phrenic nerves, one on each side. If only one side is affected, symptoms may be milder but still noticeable, especially with exertion. If both sides are involved, breathing problems can become much more severe.
How Nerve Damage Affects Breathing
When the phrenic nerve is damaged, the diaphragm may not contract fully or at all. This is sometimes called diaphragm paralysis or dysfunction. The result is reduced lung expansion, which leads to that frustrating feeling of not being able to get a full breath.
What Does Phrenic Nerve Damage Feel Like?
Phrenic nerve damage does not usually feel dramatic at first. It often builds slowly and can be subtle. But the symptoms are real and disruptive.
Shortness of Breath Without Lung Disease
Many people describe it as struggling to take a deep breath.
You may feel like you cannot fully expand your lungs, even though oxygen levels look normal on basic tests. There is often a sense of “air hunger” — like your body wants more air but cannot get it.
You might feel winded walking up stairs, bending over, or carrying groceries, even if you are otherwise healthy.
Breathing Difficulty When Lying Down
A classic symptom is difficulty breathing when lying flat. This is called orthopnea.
In simple terms, it means you feel more short of breath when you lie on your back. When you are flat, gravity no longer helps your diaphragm. If the muscle is weak, breathing can feel more restricted.
Many people end up sleeping propped up on pillows without realizing why.
Chest Tightness or Pressure
Phrenic nerve dysfunction can cause chest discomfort that feels serious. It may feel like tightness or pressure.
Importantly, this discomfort is not cardiac in origin. Heart tests are often normal. Because of that, symptoms are sometimes labeled as anxiety. While anxiety can worsen breathing sensations, it is not always the root cause.
Persistent Fatigue
When your diaphragm is not working efficiently, oxygen exchange can be reduced. Even small inefficiencies add up over time.
The result is persistent fatigue. You may feel drained after minor activity. Sleep can also suffer, especially if breathing is compromised at night.
Reduced Exercise Tolerance
One of the most frustrating symptoms is decreased stamina.
Climbing stairs may feel unusually hard. Light workouts may leave you wiped out. You might feel weak during physical activity, even though your muscles themselves are not injured.
It is not a lack of effort. It is a breathing limitation driven by nerve dysfunction.
Why Phrenic Nerve Damage Is Often Misdiagnosed
One of the most frustrating parts of phrenic nerve dysfunction is that standard tests often look normal.
Normal Cardiac and Pulmonary Testing
Heart tests are fine.
Lung scans look okay.
Oxygen levels may even appear normal at rest.
Because of that, patients are often told nothing serious is wrong. But normal heart and lung tests do not rule out a nerve problem affecting the diaphragm.
Symptoms Often Mistaken For Something Else
Phrenic nerve issues commonly get labeled as:
- Anxiety – because shortness of breath and chest pressure overlap with panic symptoms.
- Asthma – especially when breathing feels restricted.
- Deconditioning – when fatigue and low stamina are blamed on lack of fitness.
While those conditions are real, they are not always the root cause. If the diaphragm is not contracting properly due to nerve dysfunction, no amount of reassurance or inhalers will fix it.
The Importance of a Nerve-Focused Evaluation
When breathing symptoms do not match test results, the nervous system needs to be considered. A nerve-focused evaluation looks beyond the lungs and heart and asks a different question: is the signal to the diaphragm functioning correctly?
That shift in thinking can change everything.
What Causes Phrenic Nerve Damage?
Phrenic nerve dysfunction can happen for several reasons. Sometimes the cause is obvious. Sometimes it is not.
Surgical Trauma
Procedures involving the neck, chest, heart, or upper spine can irritate or injure the phrenic nerve. Even carefully performed surgeries carry some risk because of how close this nerve travels to major structures.
Cervical Spine Issues
Since the phrenic nerve starts at C3 to C5, problems in the cervical spine such as disc herniations, degeneration, or spinal stenosis can affect the nerve roots.
Viral Inflammation
Certain viral infections can trigger nerve inflammation. In some cases, breathing changes begin after a respiratory illness and never fully resolve.
Tumors or Masses
Growths in the chest or neck can compress the nerve. This is less common but important to rule out.
Idiopathic Cases
Sometimes no clear cause is found. Symptoms develop gradually without a specific injury or event. These cases are often labeled idiopathic, meaning the exact reason is unknown.
Chronic Compression or Irritation
Long-standing mechanical pressure, posture-related issues, or scar tissue can irritate the nerve over time, leading to dysfunction rather than sudden paralysis.
When Should You Seek Medical Evaluation?
Not every episode of shortness of breath is serious. But certain patterns deserve attention.
You should seek evaluation if you notice:
- Shortness of breath without a clear cause, especially when heart and lung tests are normal
- An elevated diaphragm on imaging, even if no one explains what it means
- Symptoms that worsen when lying down
- Ongoing fatigue despite a normal cardiac and pulmonary workup
If something feels off and you are not getting answers, it is reasonable to dig deeper. Persistent symptoms are not something you should simply learn to live with.
At that point, a specialist experienced in nerve-related dysfunction can help determine whether the issue is structural, inflammatory, or neurologic.
How is Phrenic Nerve Dysfunction Diagnosed?
Diagnosis usually involves putting several pieces together.
Physical Exam
Doctors may look for breathing asymmetry, reduced chest expansion, or signs of muscle weakness. Sometimes subtle findings during a routine exam raise suspicion.
Imaging
Imaging can show diaphragm elevation or abnormal movement.
- Chest X-ray may reveal one side sitting higher than the other.
- Ultrasound can assess diaphragm movement in real time.
- Fluoroscopy evaluates how the diaphragm moves during breathing.
These tests help determine whether the muscle is functioning properly.
Pulmonary Function Testing
Breathing tests measure lung capacity and airflow. Certain patterns, especially changes when lying down, can suggest diaphragm weakness.
Nerve Conduction Studies
In some cases, specialized testing evaluates how well electrical signals travel along the nerve. These studies help determine whether the nerve itself is impaired.
Treatment Options for Phrenic Nerve Damage
Treatment depends on severity, cause, and how much function remains.
Conservative Management
For mild cases, non-surgical strategies may help.
Breathing Exercises
Targeted breathing techniques can strengthen accessory muscles and improve efficiency.
Physical Therapy
Postural work and core strengthening may reduce mechanical strain on the nerve.
Monitoring Mild Cases
If function is partially intact, doctors may monitor symptoms over time to see if spontaneous recovery occurs.
Interventional or Surgical Options
In more severe cases, especially with diaphragm paralysis, advanced treatments may be considered.
Nerve Repair or Reconstruction
Specialized procedures may attempt to restore nerve continuity or function when structural damage is identified.
Diaphragm Pacing
In certain situations, devices can stimulate the diaphragm to contract. This is typically reserved for select cases and evaluated carefully.
Multidisciplinary Evaluation
Management often involves coordination between pain specialists, neurologists, pulmonologists, and surgeons. The goal is accurate diagnosis first, then thoughtful treatment planning.
This is not about rushing to surgery. It is about identifying the correct cause and matching the right intervention.
Can Phrenic Nerve Damage Improve?
Improvement depends on several factors.
It Depends on the Cause
Inflammatory or temporary compression cases may improve over time. Structural injuries are less likely to resolve on their own.
Partial vs Complete Injury
Partial nerve injury has a better chance of recovery than complete paralysis. Preserved signal function improves prognosis.
Early Diagnosis Matters
The sooner dysfunction is identified, the more options exist. Delayed diagnosis can allow muscle weakening and secondary complications to progress.
Conclusion: When Breathing Symptoms Shouldn’t Be Ignored
If you are experiencing unexplained shortness of breath, fatigue, or chest tightness and your tests keep coming back normal, that does not mean nothing is wrong.
Nerve-related causes of breathing difficulty are often overlooked. The phrenic nerve plays a critical role in diaphragm function, and when that signal is disrupted, symptoms can be real and persistent.
If you are dealing with complex nerve-related pain or dysfunction, Dr. Shane Huch, a pain management doctor in New Jersey, evaluates patients with difficult-to-diagnose neurologic conditions