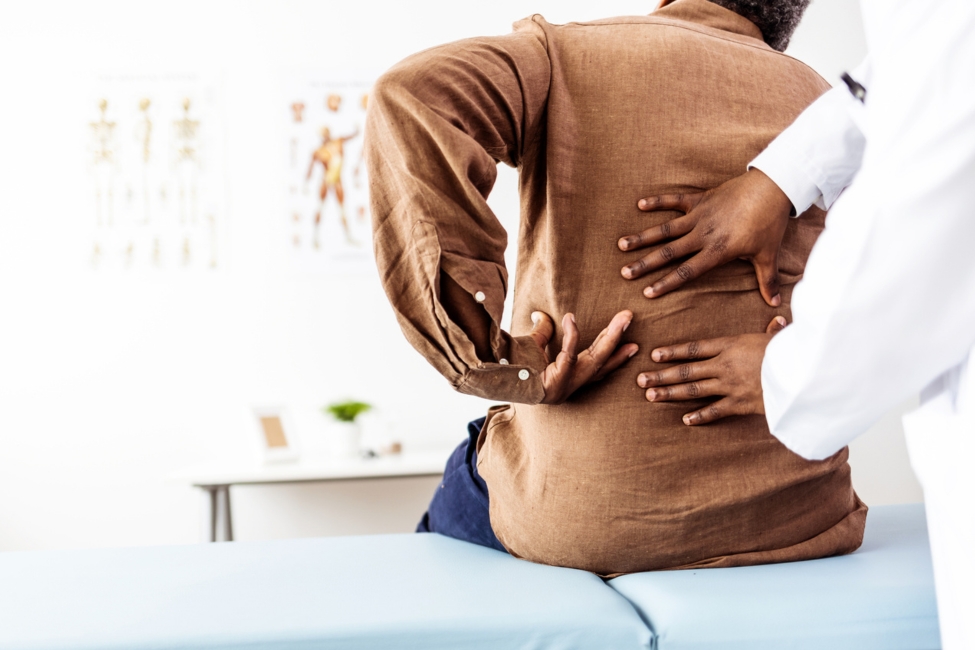
A “locked up” back usually means the muscles around your spine have suddenly tightened or gone into spasm. It can cause sharp pain, stiffness, difficulty standing upright, or the feeling that your back is stuck and every movement might make it worse.
If your back keeps locking up, it may be time to explore pain management New Jersey options to find out what is triggering the problem. Repeated episodes can sometimes point to underlying spinal irritation, disc issues, joint stress, nerve irritation, or instability that should be evaluated.
What Does It Mean When Your Back “Locks Up”?
The muscles tighten to protect the spine
When your back locks up, your muscles may be reacting to something they see as a threat. This can happen when a joint, disc, nerve, ligament, or muscle becomes irritated.
The spasm is often protective. Your body tightens the surrounding muscles to limit movement and prevent more irritation. That is why the pain can feel sudden and intense, even if the movement that caused it seemed small.
The problem is that this protective tightening can also create a temporary loss of mobility. Your back may feel stiff, guarded, and difficult to move.
Back spasms can happen suddenly
A locked back does not always happen during heavy lifting. Sometimes it happens during simple, everyday movements.
Common triggers include:
- Turning over in bed
- Getting out of a car
- Bending forward
- Twisting the spine
- Picking up or lifting objects
- Standing up after sitting too long
Often, the movement catches your body off guard. If the spine is already irritated or the muscles are already tight, one small motion can trigger a larger spasm.
The back may feel stiff, seized, or stuck
When your back locks up, it may feel like your body is refusing to move normally. You may have trouble standing upright, walking smoothly, or changing positions.
Some people lean to one side or stay bent forward because standing straight increases the pain. This is often part of muscle guarding. Your body is trying to avoid the position that feels most painful.
The pain may feel sharp with movement, then settle into a deep stiffness or cramping when you stay still.
Common Causes of a Locked Up Back
Muscle strain or overuse
A muscle strain can happen when the back muscles are stretched, overloaded, or used beyond what they can handle. This may come from lifting, exercise, yardwork, awkward movement, or repetitive strain.
When the muscle fibers become irritated, the surrounding muscles may tighten to protect the area. This can create the locked-up feeling and make simple movement painful.
Herniated discs or disc irritation
Spinal discs sit between the bones of the spine and help absorb pressure. If a disc becomes irritated, bulges, or herniates, nearby nerves and tissues may become sensitive.
The muscles around the spine may spasm to protect the irritated area. This can cause sudden lower back pain, stiffness, difficulty standing upright, and sometimes pain that travels into the buttock or leg.
Joint irritation in the spine
The small joints in the spine help guide movement. When these joints become irritated, inflamed, or compressed, the surrounding muscles may tighten.
This can happen after twisting, bending, poor posture, or repeated stress. The back may feel locked because the muscles are trying to limit movement around the irritated joint.
Weak core and spinal stabilizing muscles
The deeper muscles around the spine help support and control movement. When these stabilizing muscles are weak, tired, or not coordinating well, the spine may rely more heavily on larger surface muscles.
That extra stress can make the back more vulnerable to spasms. If the body feels unstable during movement, it may tighten suddenly to protect the spine.
Poor posture and prolonged sitting
Sitting for long periods can place stress on the lower back, especially when posture is slumped or unsupported. Over time, this can irritate muscles, discs, and joints.
When you finally stand, bend, or twist, the back may react sharply. A locked-up episode can happen because the tissues were already stiff and sensitive before the movement occurred.
Sudden twisting or awkward movement
A quick twist, reach, or awkward bend can trigger a back spasm, especially if the spine is not prepared for the movement.
This can happen while grabbing something from the floor, turning while lifting, stepping wrong, or moving quickly after being still. The muscles tighten because the body senses stress around the spine.
Stress and muscle tension
Stress can increase muscle tension throughout the body, including the back. When the muscles stay tight for long periods, they may become more prone to spasms.
Stress alone may not be the only cause, but it can make an irritated back more reactive. Tight muscles, shallow breathing, poor sleep, and prolonged tension can all make flare-ups more likely.
Why Back Muscles Go Into Spasm
Muscle spasms are often protective
A back spasm is usually the body’s attempt to protect itself. When the spine feels irritated or unstable, the muscles tighten to prevent movement that could make things worse.
This can help stabilize the area temporarily, but it can also make the pain feel more intense. The tighter the muscles become, the harder it is to move comfortably.
That is why a locked back can feel scary. The body is limiting movement, but the protection itself becomes painful.
Inflammation can trigger muscle tightening
Inflammation is another common reason the back locks up. If a disc, joint, nerve, ligament, or muscle becomes inflamed, the surrounding muscles may react by tightening.
Disc inflammation may cause deep lower back pain or symptoms into the leg. Joint irritation may cause localized stiffness or sharp pain with certain movements. Nerve irritation may cause pain that travels, tingles, burns, or feels electrical.
The muscles around the irritated area tighten as part of the body’s response.
The nervous system increases muscle tension
Pain signals can cause the nervous system to increase muscle tension. This is called guarding.
Guarding is meant to protect the painful area, but it can also create a cycle. Pain causes tightness, tightness limits movement, limited movement increases stiffness, and stiffness can make the pain feel worse.
Breaking that cycle usually starts with understanding what triggered the spasm in the first place.
Symptoms That Often Happen With a Locked Back
Sharp lower back pain
A locked back often starts with a sudden, sharp pain in the lower back. It may happen during a simple movement, like bending forward, standing up, twisting, or getting out of bed.
The pain can feel intense because the muscles around the spine tighten quickly. Even small movements may feel risky or painful at first.
Difficulty standing or walking normally
When your back locks up, standing upright may feel almost impossible. You may feel stuck in a slightly bent position or feel like your back will spasm again if you try to straighten.
Walking may also feel awkward. Your steps may become shorter, slower, or uneven because your body is trying to avoid triggering more pain.
Pain when changing positions
Changing positions is often one of the hardest parts of a locked back episode. Rolling over in bed, getting out of a chair, standing from a seated position, or getting into a car may all cause pain.
This happens because position changes require the spine, hips, and core muscles to work together. When the back is in spasm, those movements can feel restricted and painful.
Muscle tightness and stiffness
A locked back usually comes with noticeable tightness. The muscles may feel hard, cramped, or tense.
This stiffness is part of the protective guarding response. Your body is trying to limit movement around an irritated area, but that same tightening can make the back feel even more stuck.
Leaning to one side
Some people notice they lean to one side when their back locks up. This can happen because the body is trying to shift away from the painful area.
Leaning, hunching forward, or standing unevenly may temporarily reduce pressure on irritated spinal structures. However, if this posture lasts or keeps returning, it may be a sign that the underlying cause should be evaluated.
Pain radiating into the buttock or leg
If pain travels into the buttock, hip, thigh, or leg, a nerve may be involved. This can happen when irritation near the spine affects a nerve pathway.
Radiating pain may feel sharp, burning, tingling, or electric. It may also suggest conditions like sciatica, disc irritation, or spinal stenosis.
When Back Locking May Be More Serious
Pain traveling into the leg
Back pain that travels down the leg can point toward nerve irritation. This does not always mean something severe is happening, but it does mean the issue may be more than a simple muscle spasm.
If leg pain is frequent, worsening, or paired with numbness or weakness, it should be evaluated.
Numbness or tingling
Numbness, tingling, pins and needles, or burning sensations may suggest that a nerve is being irritated or compressed.
These symptoms may show up in the buttock, leg, foot, toes, arm, or hand, depending on where the nerve irritation is happening. Persistent or spreading numbness should not be ignored.
Weakness in the legs
Leg weakness is more concerning than pain alone. If your leg feels heavy, unstable, hard to lift, or weaker than usual, a nerve may not be functioning properly.
Weakness should be evaluated promptly, especially if it is new, worsening, or affecting walking, balance, or stairs.
Loss of bladder or bowel control
Loss of bladder or bowel control with severe back pain is an emergency symptom. It may point to serious nerve compression and needs immediate medical attention.
Other emergency signs may include numbness in the groin or saddle area, severe leg weakness, or sudden loss of sensation. These symptoms should not wait for a routine appointment.
Symptoms that keep returning
If your back locks up once and improves, it may have been a temporary strain or flare-up. But if it keeps happening, there may be an underlying issue that is not fully resolving.
Recurring back spasms may be connected to disc irritation, joint inflammation, nerve compression, muscle imbalance, poor movement patterns, or spinal instability. An evaluation can help identify the source before the episodes become more frequent.
What to Do When Your Back Locks Up
Short periods of rest
A short period of rest can help calm severe pain at the beginning of a back spasm. The key word is short.
Resting for a little while may help the muscles relax, but staying completely inactive for too long can make stiffness worse. Once the sharp pain begins to settle, gentle movement is usually better than prolonged bed rest.
Gentle movement and walking
Gentle movement can help keep the back from tightening further. Short, easy walks may improve circulation, reduce stiffness, and help the muscles gradually relax.
The goal is not to force big movements or push through severe pain. Start small and move within a comfortable range.
Ice and heat therapy
Ice may help during the early phase if the area feels inflamed or sharply painful. Heat may help later when the main issue is tightness, stiffness, or muscle guarding.
Some people respond better to one than the other. The goal is to reduce discomfort, calm irritation, and help the muscles relax enough to move more comfortably.
Positioning that reduces stress on the spine
Certain positions may reduce pressure on the lower back. Lying on your back with pillows under your knees can help some people. Others feel better lying on their side with a pillow between the knees.
The right position is usually the one that allows your muscles to settle and your pain to calm down. Avoid positions that increase leg pain, numbness, or sharp spasms.
Avoiding prolonged inactivity
It is natural to want to avoid movement when your back locks up, but too much inactivity can make the back stiffer.
As symptoms calm, gentle walking, light mobility, and gradual return to normal activity can help prevent the spasm cycle from dragging on. Avoid heavy lifting, twisting, or aggressive stretching until the back feels more stable.
Non-Surgical Treatment Options for Recurring Back Spasms
Physical therapy
Physical therapy can help identify movement patterns, weakness, stiffness, or instability that may be contributing to recurring spasms.
Treatment may include mobility work, strengthening, posture training, core control, and safer movement mechanics. The goal is to reduce strain on the spine and make future flare-ups less likely.
Epidural steroid injections
If back locking is connected to nerve inflammation from a disc issue, spinal stenosis, or sciatica, an epidural steroid injection may be considered.
This treatment places anti-inflammatory medication near irritated spinal nerves. The goal is to reduce inflammation, calm radiating pain, and help improve function without surgery.
Nerve blocks
Nerve blocks may be used when a specific nerve or joint-related pain source is suspected. They can help reduce pain signals and may also help confirm where the pain is coming from.
This can be useful when symptoms keep returning and the exact source is unclear.
Radiofrequency ablation
Radiofrequency ablation may be an option when certain spinal joints or nerves are repeatedly contributing to pain.
This procedure uses controlled heat energy to interrupt targeted pain signals. It is typically considered after diagnostic injections suggest the involved nerves are the likely pain source.
Core strengthening and movement retraining
Recurring back spasms often improve when the spine has better support. Core strengthening is not just about doing more sit-ups. It means training the deep stabilizing muscles to support the spine during real movement.
Movement retraining can also help you bend, lift, sit, stand, and twist with less stress on irritated areas. Over time, this can reduce the chance of future flare-ups.
Understanding Why Your Back Locks Up Can Help You Prevent Future Flare-Ups
Back locking is often a protective muscle spasm. Your body tightens the muscles around the spine to limit movement and protect an irritated area.
The underlying irritation may involve discs, joints, nerves, muscle strain, or poor spinal stability. That is why persistent or recurring symptoms should be evaluated instead of brushed off as “just a bad back.”
If you keep dealing with recurring back spasms, radiating pain, numbness, or severe stiffness, exploring pain management New Jersey options can help identify the source and guide a non-surgical treatment plan
Frequently Asked Questions About Back Flare Ups
Why does my back suddenly lock up?
Your back may suddenly lock up when muscles tighten to protect an irritated area of the spine, such as a strained muscle, inflamed joint, irritated disc, or compressed nerve.
Can a herniated disc make your back seize up?
Yes. A herniated or irritated disc can trigger nearby muscles to tighten protectively, which may make the back feel seized, stiff, or stuck.
How long does a back spasm last?
Some back spasms improve within a few days, while others may last longer depending on the cause. Spasms that persist or keep returning should be evaluated.
Why can’t I stand up straight when my back locks up?
You may not be able to stand straight because the muscles are guarding the painful area. Your body may lean or bend to reduce pressure on irritated tissues.
Is a locked back serious?
A locked back is not always serious, but it should be evaluated if pain travels into the leg, symptoms include numbness or weakness, or episodes keep returning.
Should I rest or move when my back locks up?
A short period of rest may help at first, but prolonged inactivity can make stiffness worse. Gentle movement and walking are often helpful once severe pain begins to calm.
When should I see a doctor for back spasms?
You should see a doctor if spasms persist, worsen, return often, radiate into the leg, or come with numbness, tingling, weakness, or bladder or bowel changes.