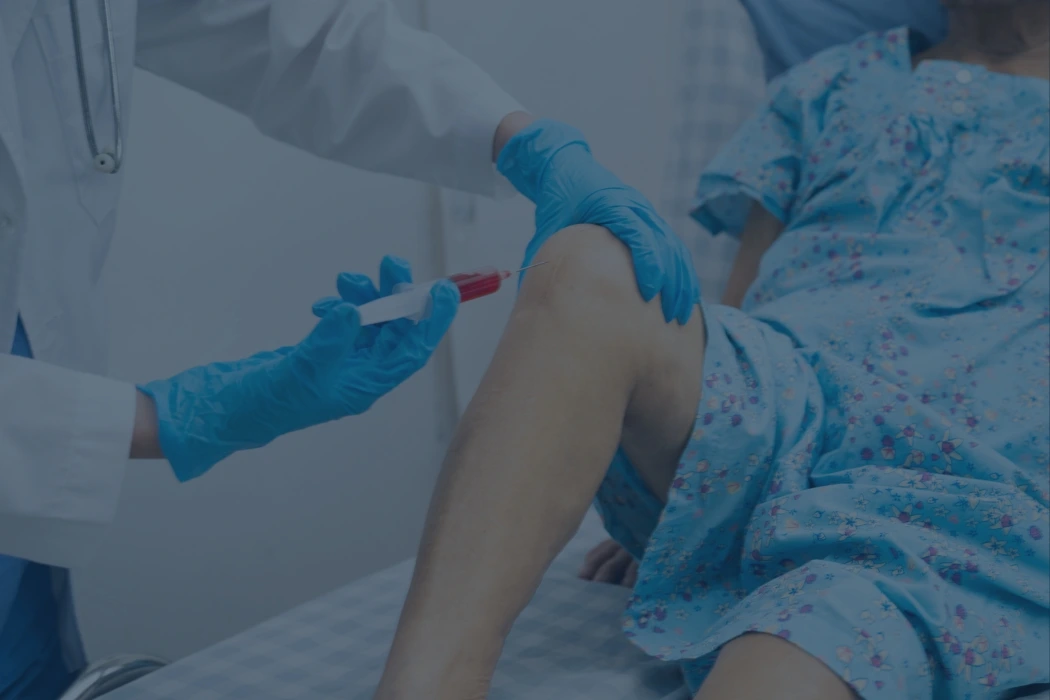
Pain injections can feel like a big step, especially if you are not sure what is being injected, why it is being recommended, or what happens afterward. That hesitation is completely normal.
If you are dealing with ongoing pain and unsure whether an injection is the right move, our team offers personalized pain management in New Jersey focused on getting to the root of the problem first. Schedule a consultation with the Center for Regenerative Therapy and Pain Management to explore treatment options that are built around your condition, not a one-size-fits-all approach.
Why Asking Questions Before an Injection Matters
Not all injections are the same. A steroid injection, nerve block, joint injection, and regenerative injection can all serve different purposes.
Asking questions helps make sure the treatment matches your diagnosis, symptoms, and long-term goals. It also helps you understand whether the injection is meant to reduce inflammation, calm irritated nerves, improve function, or support healing.
Most importantly, it sets realistic expectations. Injections may provide meaningful pain relief, but they are not always a permanent cure. Some patients feel better quickly, while others need more time, additional treatment, or a different approach.
What Type of Injection Is This?
Before agreeing to an injection, ask exactly what kind it is. Different injections are used for different reasons.
A few common examples include:
- Steroid injections: Often used to reduce inflammation around joints, nerves, or the spine.
- Nerve blocks: Used to interrupt pain signals and help identify or treat nerve-related pain.
- Regenerative injections: May be used to support the body’s natural healing response in certain soft tissue, joint, or injury-related conditions.
You should also ask where the injection is going. Is it being placed into a joint, near a nerve, around the spine, or into a soft tissue area? The location matters because it affects the goal, technique, recovery, and expected outcome.
A good follow-up question is: “Why are you recommending this specific injection for me?”
What Condition Is This Treating?
A clear diagnosis matters. An injection should not be recommended just because something hurts.
For example, low back and leg pain may be related to a herniated disc, spinal stenosis, arthritis, muscle irritation, or nerve inflammation. Knee pain may come from arthritis, tendon injury, ligament strain, or another joint issue.
If the source of pain is unclear, the injection may not help as much as expected. That is why patients should ask what condition is being treated and how that diagnosis was confirmed.
Helpful questions include:
- “What do you think is causing my pain?”
- “Do my exam or imaging results support this injection?”
- “Are we treating the root cause or only the symptoms?”
What Results Should I Realistically Expect?
Ask what the injection can and cannot do. This is where many patients get disappointed because they expect full recovery when the realistic goal may be pain reduction.
Some injections are meant to calm inflammation. Others may help confirm where pain is coming from. Some may reduce pain enough for you to move better, sleep better, or participate in physical therapy.
You should ask:
- “How much pain relief is realistic?”
- “How long might the relief last?”
- “What percentage of patients with my condition usually respond?”
- “What would count as a good result?”
For some steroid injections, relief may last days, weeks, or months depending on the condition and the patient. Cleveland Clinic notes that epidural steroid injections may start working within two to seven days, with relief lasting from several days to months in some cases.
How Long Will It Take to Work?
Some injections work quickly. Others take several days or longer.
You may feel temporary numbness or early relief if a local anesthetic is used. That does not always mean the full treatment has worked yet. With steroid injections, it is also possible for soreness or pain to briefly increase before improvement begins.
Ask your provider what timeline is normal for your specific injection.
You should also ask what is not normal. Worsening pain, signs of infection, fever, new weakness, or numbness that does not improve should be reported right away. Cleveland Clinic recommends contacting a provider after certain spinal injections if numbness or weakness lingers, new pain appears, existing pain worsens, or signs of infection develop.
How Many Injections Will I Need?
Some patients only need one injection. Others may need a series, depending on the diagnosis and how they respond.
This is especially important with steroid injections. Repeated steroid use can carry additional risks, so you should ask how often the injection can safely be repeated and when it would make sense to stop. Mayo Clinic lists potential risks of cortisone shots including cartilage damage, joint infection, nerve damage, short-term blood sugar increases, tendon weakening, and skin or soft tissue changes.
Good questions include:
- “Is this a one-time injection or part of a series?”
- “How long should we wait before deciding if it worked?”
- “How many injections are safe for this area?”
- “At what point do we change the treatment plan?”
What Are the Risks or Side Effects?
Every procedure has some level of risk. That does not mean injections are unsafe for everyone, but it does mean you should understand the possible downsides.
Common side effects may include temporary soreness, swelling, bruising, or increased pain for a short period after the injection. Less common risks may include infection, bleeding, allergic reaction, or nerve irritation.
Steroid injections may also have specific concerns, especially with repeated use or certain health conditions. Hospital for Special Surgery notes that corticosteroids can raise blood sugar and may affect blood pressure in some patients.
Ask your provider:
- “What side effects are most common with this injection?”
- “What risks apply to my health history?”
- “What symptoms should make me call your office?”
- “Are there any reasons I should avoid this injection?”
Are There Alternatives to This Injection?
An injection may be the right choice, but it should not feel like the only choice unless your provider clearly explains why.
Alternatives may include:
- Physical therapy
- Activity modification
- Anti-inflammatory medications
- Bracing or support
- Regenerative treatments
- Lifestyle changes
- Additional diagnostic testing
- Surgery in more severe cases
Sometimes injections are used after conservative care has not helped. Other times, they are used earlier because pain is limiting movement, sleep, or daily function.
Ask: “What would you recommend if I did not choose the injection today?”
What Happens If I Don’t Get the Injection?
This is one of the most important questions because it helps you understand urgency.
Some injections are optional and focused on symptom relief. Others may be recommended because pain is limiting your recovery or because inflammation is affecting your ability to function.
Ask whether waiting could make the condition worse, or whether you have time to try other options first. This can help you avoid feeling pressured into a decision before you understand the bigger picture.
Helpful questions include:
- “Is this time-sensitive?”
- “What happens if I wait?”
- “Can I try another option first?”
- “Is there a risk of the condition getting worse without treatment?”
Who Is Performing the Injection?
Experience matters. The provider should understand the anatomy, diagnosis, imaging, and technique involved.
You should also ask whether the injection will be guided by imaging, such as fluoroscopy or ultrasound. Image guidance can help the provider place the medication more precisely, especially for spine, joint, or nerve-related injections.
Ask:
- “Who will perform the injection?”
- “How often do you perform this type of procedure?”
- “Will imaging guidance be used?”
- “Why is this approach best for my condition?”
Precision matters because the goal is not just to “give a shot.” The goal is to place the treatment in the right area for the right reason.
What Should I Do Before and After the Injection?
Your provider should give clear instructions before and after the procedure. Following those instructions can help reduce risk and improve your recovery.
Before the Injection
Ask whether you need to stop any medications before the procedure, especially blood thinners, anti-inflammatory medications, or supplements that may affect bleeding risk. Never stop prescribed medication without direct medical guidance.
You should also ask about eating, drinking, transportation, and whether you can drive yourself home. Some injections may require someone to drive you, especially if sedation is used or if the procedure may temporarily affect strength or sensation.
After the Injection
Ask what activities you should avoid and when you can return to normal movement, work, exercise, or physical therapy.
You should also ask when to expect results. Some soreness may be normal, but certain symptoms should be reported quickly, including fever, worsening redness, increasing swelling, severe new pain, or new neurological symptoms.
How Will We Measure If It Worked?
Pain relief is important, but it should not be the only measurement.
A successful injection may help you walk farther, sit longer, sleep better, reduce medication use, return to therapy, or move with less limitation. These functional improvements matter because the real goal is improving your daily life.
Before the injection, ask your provider what success should look like.
You may want to track:
- Pain level before and after
- How long relief lasts
- Walking tolerance
- Sitting or standing tolerance
- Sleep quality
- Ability to work, exercise, or complete daily tasks
- Need for pain medication
If the injection does not work, ask what happens next. A lack of relief may mean the treatment needs more time, the diagnosis needs to be reconsidered, or another treatment option may be a better fit.
When Is an Injection the Right Choice?
An injection may be the right choice when your pain has not improved with more conservative care. That may include rest, physical therapy, activity changes, anti-inflammatory medication, or other non-surgical treatments.
It may also make sense when pain is seriously limiting daily life. If you cannot walk comfortably, sleep through the night, sit at work, exercise, or handle normal routines, an injection may help reduce pain enough to get you moving again.
The key is diagnosis. An injection should match the condition being treated. If the diagnosis supports the injection, and your symptoms line up with that diagnosis, the treatment decision becomes much clearer.
Common Mistakes Patients Make
Patients do not need to know every medical detail before getting an injection, but they should understand the basics. These are a few common mistakes to avoid.
Jumping Into Injections Too Quickly
Some people agree to an injection before they fully understand why it is being recommended. Injections can be helpful, but they should be part of a thoughtful treatment plan, not a rushed next step.
Not Understanding the Diagnosis
Pain is a symptom, not a diagnosis. Before getting an injection, you should know what condition is being treated and why that injection fits your situation.
Expecting Permanent Results
Some injections provide long-lasting relief, but many are designed to reduce pain, calm inflammation, or improve function for a period of time. They may help you move better and participate in rehab, but they are not always a permanent fix.
Not Asking About the Follow-Up Plan
The injection should not be the whole plan. Ask what happens after the procedure, how results will be measured, and what the next step is if it works or does not work.
Questions to Ask: Quick Checklist
Before your appointment, keep these questions handy:
- What type of injection are you recommending?
- What condition is this treating?
- Why is this injection the right option for me?
- What results should I realistically expect?
- How long will it take to work?
- How long might the relief last?
- How many injections might I need?
- What are the risks or side effects?
- Are there alternatives I should consider first?
- What happens if I wait?
- Who will perform the injection?
- Will imaging guidance be used?
- What should I do before the procedure?
- What should I avoid afterward?
- How will we measure whether it worked?
- What is the follow-up plan?
Final Thoughts
Injections can be effective when they are used for the right condition, at the right time, and as part of a bigger treatment plan. They may help reduce pain, improve movement, and make daily life more manageable.
But the decision should be informed, not rushed. The more you understand the purpose, risks, alternatives, and follow-up plan, the more confident you can feel about your care.
Schedule a Consultation
At the Center for Regenerative Therapy and Pain Management, we take a diagnosis-first approach. That means we do not recommend injections just to recommend injections.
If you are considering an injection and want clear answers before making a decision, our team provides personalized pain treatment in New Jersey focused on real diagnosis and long-term results. Connect with a trusted pain management provider in New Jersey at Center for Regenerative Therapy and Pain Management to explore the right next step for your condition.