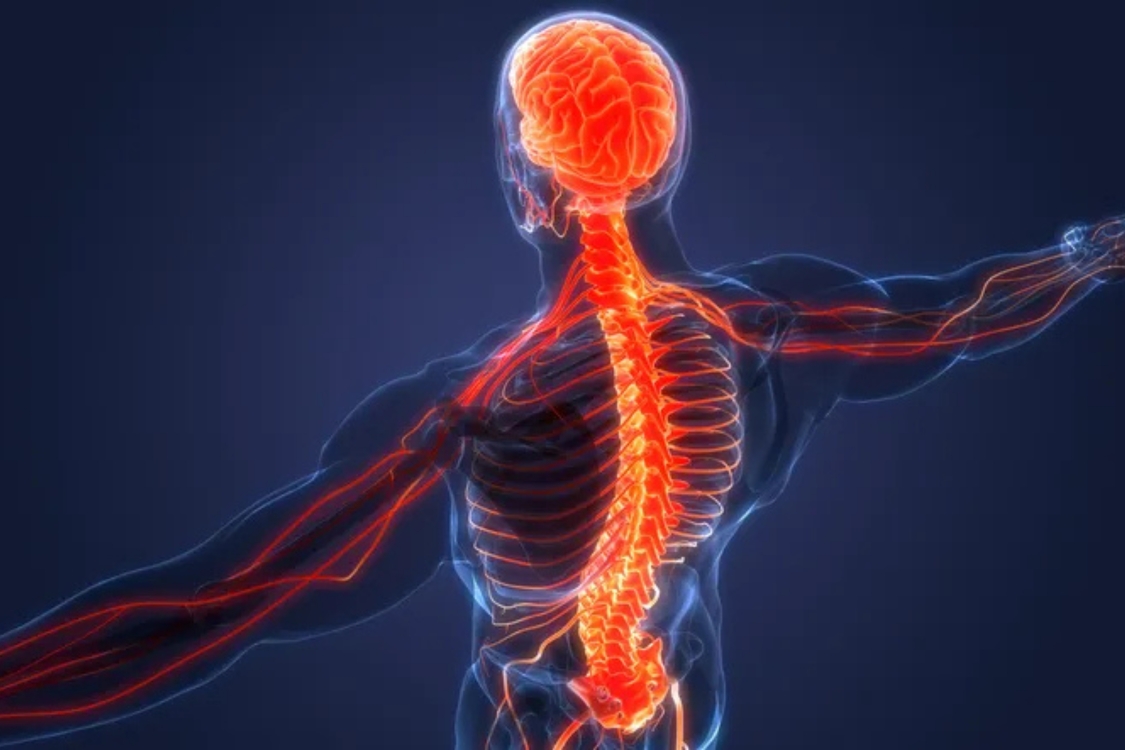
Pain is not just a feeling. It is a process that starts in the body, moves through the nerves and spinal cord, and is finally interpreted by the brain. This happens very quickly and often automatically, which is why you can pull your hand away from something hot before you even fully think about it.
Pain is important because it helps protect the body, but it can also become a problem when the signals keep firing longer than they should. In this guide, we will break down how pain signals work step by step, why pain can feel different from person to person, and what happens when the system stops working normally.
If you are dealing with ongoing or unexplained pain, our New Jersey pain management team can help identify the source and provide targeted treatment options.
What is a Pain Signal?
A pain signal is the body’s way of sending a message to the brain that something may be wrong. That message can be triggered by injury, inflammation, pressure, or nerve irritation. In simple terms, pain is a communication system between the body and the brain.
Pain as a warning system
Pain is designed to protect you. If you twist your knee, burn your hand, or irritate a nerve, pain tells you to stop, adjust, or get help. Without pain, it would be much harder to recognize injury before it gets worse.
Types of pain signals (acute vs chronic)
Acute pain signals usually happen right after an injury or clear problem. They are short term and often improve as the body heals. Chronic pain signals last much longer and may continue even after the original injury has improved. This is when pain becomes more than a normal warning sign.
Why pain is necessary
Pain is unpleasant, but it serves a purpose. It helps limit movement, protect injured tissue, and push you to pay attention to a problem. The issue is not pain itself. The issue is when pain keeps going when it no longer serves that protective role.
Step-by-Step: How Pain Signals Travel Through the Body
Pain signals move through the body in a sequence. The process is fast, but each step matters.
Step 1: Injury or stimulus occurs
The process starts when something affects tissue in the body. This could be tissue damage, inflammation, pressure, heat, or irritation. It does not always have to be a major injury. Even swelling or joint irritation can start the signal.
Step 2: Pain receptors (nociceptors) activate
Special nerve endings called nociceptors detect harmful or potentially harmful stimuli. These receptors are found in the skin, muscles, joints, and other tissues. When they detect trouble, they activate and send a message forward.
Step 3: Signals travel through nerves
Once activated, the signal travels through peripheral nerves as an electrical message. These nerves carry the information from the injured or irritated area toward the spinal cord.
Step 4: Signals reach the spinal cord
The spinal cord acts like the first processing center. It helps relay the signal upward and can also influence how strong that signal feels. This is one reason pain is not always just about the original injury. The nervous system also shapes the response.
Step 5: Signals travel to the brain
After the spinal cord, the signals travel to the brain. This is where the information is interpreted. The brain looks at the signal, compares it to past experience, and decides how serious it seems.
Step 6: Brain creates the feeling of pain
The feeling of pain happens when the brain interprets the signal as pain. This is why pain is both physical and neurological. The body sends the message, but the brain creates the actual experience. That is also why pain can feel different depending on the person, the situation, and the nervous system itself.
Types of Pain Signals
Not all pain signals are the same. Different types of pain come from different causes and often feel very different.
Nociceptive pain (tissue injury)
Nociceptive pain comes from tissue injury or inflammation. This is the kind of pain people often describe as aching, throbbing, sore, or sharp. It is common with arthritis, muscle strains, joint irritation, and many injuries.
Neuropathic pain (nerve-related)
Neuropathic pain comes from irritated or damaged nerves. It often feels burning, shooting, electric, tingling, or numb. This type of pain is common with sciatica, nerve compression, and certain spine conditions.
Referred pain
Referred pain is pain that is felt in a different place from where the actual problem starts. For example, a spine problem may cause pain in the hip or leg. This happens because the nervous system can interpret signals in ways that are not always perfectly local.
Chronic pain signals
Chronic pain signals continue over time and may keep firing even when there is no clear new injury. In these cases, the nervous system becomes part of the problem, not just the messenger.
Why Pain Can Feel Different
Pain can feel sharp, dull, burning, aching, constant, or intermittent because not all pain travels the same way. The type of tissue involved, the nerve pathway being used, and how the brain interprets the signal all affect the experience.
Different nerve pathways
Different nerve fibers carry different types of pain signals. Some send quick, sharp pain. Others carry slower, aching pain. That is one reason a fresh injury may feel different from deep joint pain or nerve pain.
Different tissues involved
Pain from muscle, joint, disc, ligament, or nerve tissue can feel very different. A joint problem may feel stiff or aching, while a nerve problem may feel burning or electric.
Brain interpretation differences
The brain does not just receive pain. It interprets it. Stress, past injuries, sleep quality, and overall nervous system sensitivity can influence how strong or how strange pain feels.
How Pain Signals Become Chronic
Pain can become chronic when the nervous system keeps sending or amplifying signals long after the original problem should have settled down. This is where the system becomes more sensitive and less efficient at turning pain off.
Pain sensitization explained
Sensitization means the nervous system becomes more reactive. Over time, smaller triggers can cause bigger pain responses. Movements that should feel normal may begin to feel painful because the system is now on high alert.
Why nerves stay “on”
Nerves can stay active when there is ongoing inflammation, repeated irritation, or long-term pressure. In some cases, the nerve itself becomes the source of the pain signal instead of just carrying it.
Why pain continues after healing
Sometimes the original tissue improves, but the nervous system keeps reacting as if the problem is still there. This is one reason chronic pain can continue after an injury appears healed on imaging or exam.
How the Brain Processes Pain
The brain plays a major role in pain. It does not just receive a signal and passively report it. It actively evaluates the signal and shapes the pain experience.
Pain perception vs actual injury
There is not always a perfect match between how much tissue damage exists and how much pain a person feels. Some people have severe pain with modest findings, while others have major structural changes and less pain. This is because pain perception involves the nervous system and brain, not just the body part itself.
Emotional and mental influence
Mood, anxiety, fear, and previous pain experiences can affect how the brain processes pain. This does not mean the pain is imaginary. It means the pain system is influenced by both physical and neurological factors.
Why stress can increase pain
Stress can increase muscle tension, inflammation, and nervous system sensitivity. When the body stays in a stressed state, pain signals may feel stronger and recovery may take longer.
Why Pain Can Spread or Change Location
Pain does not always stay in one place. It can spread, shift, or appear in nearby areas over time.
Movement changes
When something hurts, people naturally change the way they move. That compensation can put extra strain on nearby muscles and joints, leading to secondary pain in other areas.
Nerve cross-signaling
The nervous system is complex, and signals can overlap. Irritation in one area may affect nearby nerve pathways, which can make pain feel broader or less clearly defined.
Secondary pain areas
A person with hip pain may develop back pain. A person with knee pain may start feeling pain in the opposite leg. This often happens because the body adapts to avoid pain, which creates new stress patterns.
How Pain Management Targets Pain Signals
Pain management works by reducing inflammation, calming irritated nerves, and interrupting abnormal pain signaling. The goal is not only to reduce pain, but also to improve function and help the body move more normally again.
Nerve blocks
Nerve blocks place medication near a nerve to interrupt pain signals and reduce inflammation. They can also help confirm where pain is coming from.
Epidural injections
Epidural injections are commonly used when pain is coming from irritated spinal nerves. They help reduce inflammation around the nerve roots and may improve radiating pain into the arm or leg.
Radiofrequency ablation
Radiofrequency ablation uses heat to disrupt pain signals from certain nerves. It is often used when a diagnostic block shows that those nerves are involved.
Regenerative therapy
Regenerative treatments such as PRP are designed to support healing in injured tissue. By improving the condition of the tissue itself, they may help reduce the pain signals being generated.
When Pain Signals Become a Problem
Pain signals become a problem when they continue too long, feel out of proportion, or start interfering with normal life. At that point, the nervous system may be contributing to the problem instead of helping protect you.
Signs pain is not normal
Pain may not be normal when it lasts more than a few weeks, keeps returning, spreads, causes numbness or tingling, affects sleep, or limits walking, work, or daily activity.
When to seek treatment
You should seek treatment when pain is ongoing, unexplained, worsening, or interfering with life. Early care can help prevent pain from becoming more chronic and harder to treat.
Pain Treatment in New Jersey
Pain treatment today often includes interventional pain management, imaging-guided procedures, and personalized care designed to target the source of pain more precisely. Depending on the cause, treatment may include injections, nerve-based procedures, regenerative therapy, medication, or physical therapy.
If pain is affecting your daily life, our New Jersey pain management specialists can help identify the source and provide targeted treatments to reduce pain and restore function.
Frequently Asked Questions About Pain Signals
What causes pain signals in the body?
Pain signals are usually caused by injury, inflammation, pressure, or nerve irritation. These triggers activate pain receptors, which send messages through the nervous system to the brain.
How fast do pain signals travel?
Pain signals can travel very quickly through nerves, especially sharp pain signals. The exact speed depends on the type of nerve fiber carrying the message.
What nerves carry pain signals?
Peripheral nerves carry pain signals from the body to the spinal cord, where the signals are then relayed to the brain.
Why does pain feel different in different areas?
Pain feels different depending on the tissue involved, the type of nerve carrying the signal, and how the brain interprets the message.
Can pain signals be blocked?
Yes. Treatments such as nerve blocks, epidural injections, and radiofrequency ablation are designed to interrupt or reduce pain signaling.
Why does pain continue after healing?
Pain can continue after healing when the nervous system stays sensitized or when nerves continue sending signals even after the original tissue problem improves.
What doctor treats nerve pain?
Pain management specialists commonly diagnose and treat nerve pain using medication, therapy, and minimally invasive procedures.