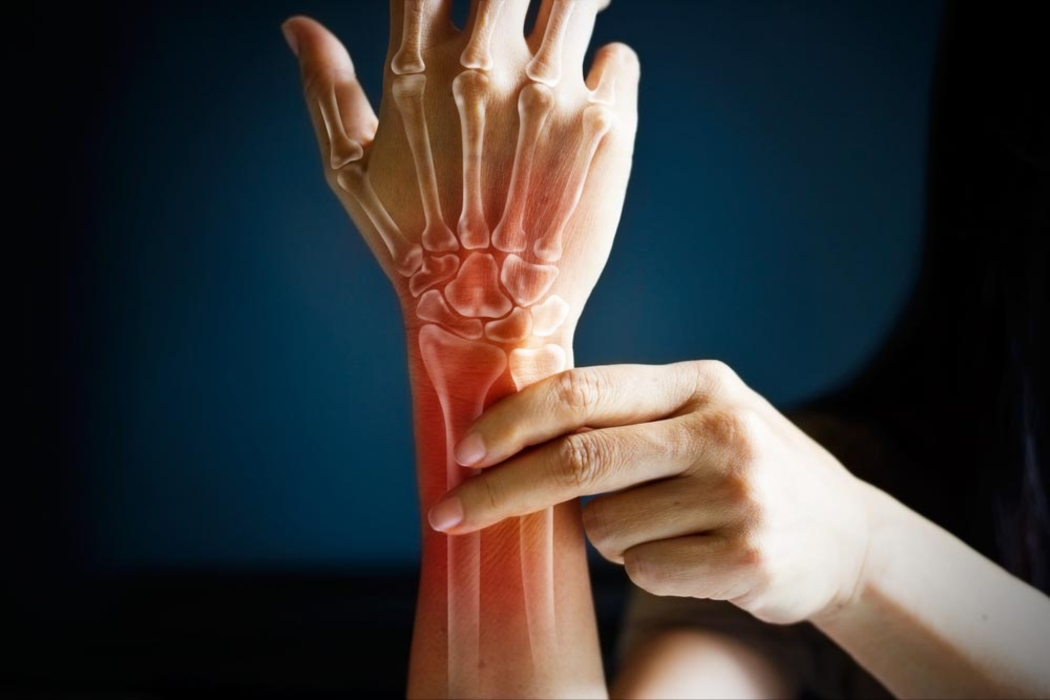
Complex regional pain syndrome (CRPS) can feel like your body hit a stuck “pain alarm” after an injury or surgery. The pain is intense, persistent, and often way out of proportion to what happened. If you want a clear diagnosis and a stepwise plan for pain management in New Jersey, schedule an evaluation early, because CRPS is one of those conditions where timing and the right approach matter.
If you’re dealing with severe limb pain, swelling, temperature or color changes, or touch sensitivity that isn’t improving, book a consultation for pain management in New Jersey to confirm the pattern and start treatment before symptoms get entrenched.
Quick Summary
The simplest definition
CRPS is a chronic pain condition, usually affecting an arm or leg, that often starts after an injury, fracture, or surgery and causes pain that’s out of proportion.
Why early care matters
CRPS is often more treatable when it’s addressed early, before long-term changes set in.
What this guide covers
Symptoms and warning signs, types of CRPS, how diagnosis works, treatment options, and what a realistic care plan looks like.
What Is Complex Regional Pain Syndrome
Plain-English definition
CRPS is when the nervous system and inflammatory response stay “turned on” after a trigger, creating ongoing pain plus sensory and skin changes.
What CRPS commonly follows
Injury or trauma, surgery, fractures, and sometimes medical events like stroke or heart attack. Sometimes people don’t remember a clear trigger.
Why the pain feels so extreme
It’s not just tissue damage. CRPS involves pain signaling, inflammation, and nervous system sensitivity interacting in a way that amplifies symptoms.
Types of CRPS: Type 1 vs Type 2
Type 1: no confirmed nerve injury
Often discussed when symptoms fit CRPS but there isn’t a clearly documented nerve injury.
Type 2: confirmed nerve injury
Similar symptom pattern, but with evidence of a distinct nerve injury.
Why the label is less important than the plan
The treatment strategy is driven by your presentation: pain behavior, function limits, and what systems seem most involved.
Symptoms of CRPS: what people actually notice
Pain features that stand out
Burning or throbbing pain, severe sensitivity to touch, pain from light contact, and pain triggered by cold.
Skin, temperature, and swelling changes
Swelling, color changes, sweating changes, and skin temperature swings. Hot and red at times, cold and pale at others.
Movement changes
Stiffness, decreased range of motion, weakness, tremor, spasms, and difficulty using the limb normally.
How symptoms can change over time
Symptoms may shift, flare, or evolve. Some people improve, some persist, and some develop more lasting changes if the limb stays guarded and immobile.
Phases and progression: what “early” vs “later” can look like
Early phase: inflammatory look
Often warmer, redder, swollen, and hypersensitive.
Later phase: stiffness and skin changes
Can become cooler, stiffer, tighter, with changes in skin texture or hair and nail growth.
The big risk: getting stuck in avoidance
When pain blocks movement, function can decline and the cycle worsens. Breaking that cycle is a major treatment goal.
What Causes CRPS: the three big drivers
Inflammation
Often a big factor early on.
Nerve injury or nerve irritation
Sometimes there’s compression, scarring, or a nerve injury component.
Sympathetic nervous system activation
The “fight or flight” system can contribute to temperature changes, sweating changes, and amplified pain.
How CRPS Is Diagnosed
Step 1: your story and timeline
What happened, when pain escalated, what changed, what makes it worse, and what makes it better.
Step 2: physical exam
Skin temperature and color changes, swelling, sensitivity, range of motion, strength, and functional limits.
Step 3: diagnostic criteria and rule-outs
CRPS is usually diagnosed clinically using structured criteria and by ruling out other explanations.
Step 4: testing when it helps the plan
Imaging and nerve studies are sometimes used to evaluate nerve involvement or exclude other causes, depending on your presentation.
Treatment Goals: what a good CRPS plan actually tries to do
Goal 1: reduce pain enough to restore movement
You don’t need zero pain to improve. You need enough control to move and rebuild function.
Goal 2: prevent stiffness and long-term disability
Keeping the limb moving safely is a big deal in CRPS.
Goal 3: calm the nervous system
This includes medication strategy, procedures when appropriate, and mind-body tools that reduce flares.
CRPS Treatment Options: what may be used and why
Medications: symptom control and signal calming
Anti-inflammatory strategies early when appropriate, neuropathic pain medications, and other meds based on the dominant driver.
Procedures: targeted options when needed
Sympathetic blocks, nerve blocks, and other interventional options can be used based on pattern and response.
Neuromodulation: when pain stays stuck
Options like peripheral nerve stimulation or spinal cord stimulation may be discussed in select cases when conservative and interventional steps aren’t enough.
Movement-based therapy: the non-negotiable
Physical and occupational therapy are core. Mirror therapy and graded motor imagery may be used to retrain the brain’s relationship with movement and sensation.
Pain psychology: reducing flare cycles
Stress management, mindfulness skills, and coping strategies can reduce nervous system reactivity and improve outcomes.
What to Expect: realistic timeline and progress markers
What progress looks like early
Less swelling, improved tolerance to touch, better range of motion, fewer flares, improved sleep.
What progress looks like later
More consistent use of the limb, better strength, less fear of movement, and improved daily function.
What can slow progress
Delayed treatment, avoiding movement completely, untreated nerve irritation, or an unclear pain generator.
When to See a Pain Specialist
Signs you should not wait on
Severe persistent limb pain after injury or surgery, touch sensitivity that feels extreme, swelling and temperature or color changes, and major function loss.
The value of early evaluation
CRPS is one of the conditions where early identification and a structured plan can change the trajectory.
Frequently Asked Questions About Complex Regional Pain Syndrome
Is CRPS permanent?
CRPS can improve, and some people experience remission, especially with early treatment. But it can also persist for months or years. The goal is to reduce pain, restore function, and prevent long-term changes.
Can CRPS go away on its own?
In some cases, symptoms improve without intensive treatment. The problem is that you can’t predict who will improve quickly, so early evaluation is still the safest move.
How is CRPS different from “normal” post-injury pain?
Normal healing pain typically improves steadily. CRPS pain tends to stay severe, spread beyond the original injury area, or come with strong sensitivity, swelling, and temperature or color changes.
What is the Budapest Criteria?
It’s a structured checklist clinicians use to support a CRPS diagnosis based on symptoms and exam findings. It helps make the diagnosis more consistent and less subjective.
What treatments help CRPS the most?
There isn’t one magic treatment. The best outcomes usually come from a combined plan: movement therapy, symptom control with medications when appropriate, targeted procedures when indicated, and strategies to reduce flare cycles.
Can CRPS spread?
It can. Some people notice symptoms extending beyond the original area or appearing in another limb. That’s another reason early treatment and movement focused care matter.
What should I do at home while waiting for an appointment?
Keep the limb gently moving within tolerance, avoid total immobilization, track symptoms and triggers, and follow any post-injury instructions you were given. If symptoms are severe or rapidly worsening, seek urgent evaluation.
Key Takeaways:
CRPS is real, complex, and often triggered after injury or surgery. Early treatment improves the odds of meaningful improvement. The best plans are multidisciplinary: movement therapy, symptom control, and targeted interventions when indicated. Function is a key outcome: pain down is great, but movement restored is the win.
If your pain feels out of proportion and your limb is changing in swelling, temperature, or sensitivity, don’t wait it out. Schedule an evaluation for pain management in NJ to confirm whether this fits CRPS and build a plan that focuses on function, flare control, and long-term recovery.